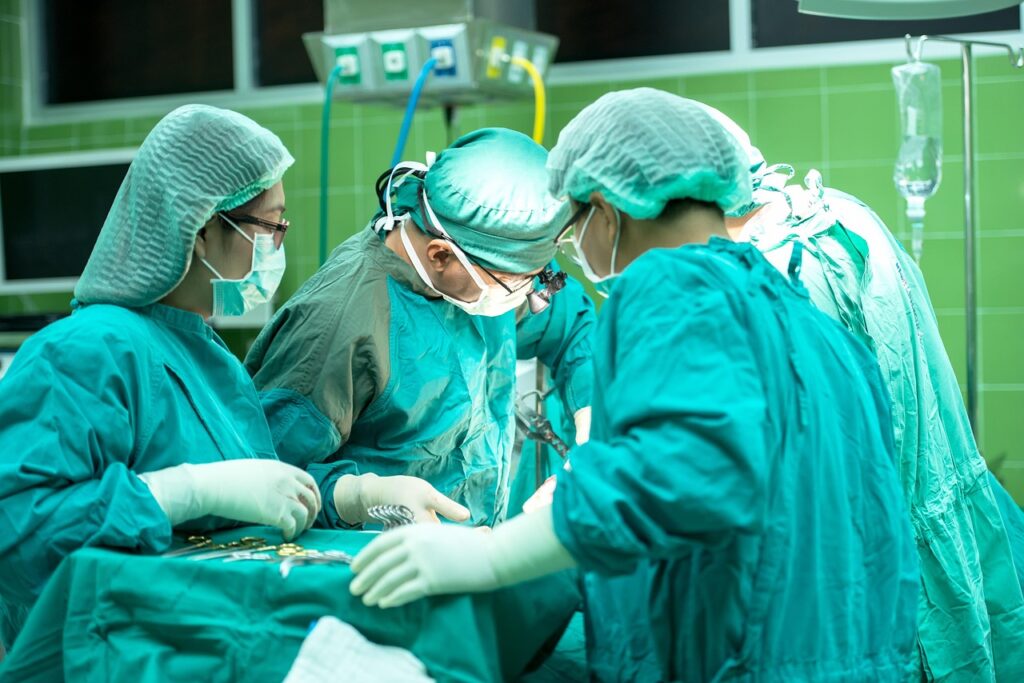
You need clear, practical guidance to navigate FDA regulatory without wasting time on guesswork. FDA regulatory consulting helps you align quality systems, regulatory strategy, and submission readiness so you can move products through development and approval more efficiently.
A good consultant translates complex rules into actionable plans for your product, whether you face clinical trial design, labeling decisions, or inspection preparedness. Expect focused support across core compliance processes and strategic services that reduce risk and keep projects on schedule.
Choosing the right partner saves resources and prevents costly delays; this article breaks down what consultants do, how they add value, and how to evaluate their fit for your program.
Core Compliance Processes
You will coordinate submission choices, compile precise regulatory files, and enforce manufacturing controls that withstand FDA inspection. These activities center on timelines, documented evidence, and demonstrable controls tied to product safety and effectiveness.
Navigating FDA Submission Pathways
Identify the correct pathway first: 510(k), De Novo, PMA, IND, NDA, or a CE route if you plan EU market entry. Choose based on device classification, risk, and available predicates.
Prepare a dossier checklist mapped to the pathway: device description, intended use, labeling, performance testing, and risk analysis. Cross-reference each item to the applicable CFR sections and FDA guidance documents.
Manage timelines with a submission project plan. Assign owners for testing, clinical evidence, and labeling updates. Track FDA interactions (pre-submission meetings, Q-sub meetings) and log written meeting minutes to reduce scope misunderstandings.
Budget for repeat testing and additional data requests. Anticipate common FDA questions and prepare modular responses to speed review.
Preparing Regulatory Documentation
Structure your submission to make review easy: a clear table of contents, indexed appendices, and trackable version control. Use consistent document identifiers, revision histories, and approved-signature pages.
Include a traceable requirements-to-test matrix that links design inputs to verification and validation results. That matrix should highlight unresolved deviations and planned mitigations.
Provide thorough risk management files per ISO 14971 and a clinical summary when human data exist. Supply complete labeling drafts and Instructions for Use (IFU) with use-related risk mitigations.
Maintain an evidence repository for raw data, test protocols, and laboratory accreditation records. Be ready to export discrete files on request and supply audit trails for electronic records.
Implementing Good Manufacturing Practices
Translate regulatory requirements into controlled processes: device history records (DHR), device master records (DMR), and work instructions. Define critical process parameters and in-process controls, and document acceptance criteria.
Establish supplier qualification and incoming inspection procedures. Record supplier audits, quality agreements, and material certificates to ensure traceability to finished product lots.
Operate a CAPA system that tracks nonconformances from detection through verification of effectiveness. Implement periodic internal audits and management reviews with measurable indicators: OOS rates, CAPA closure time, and audit findings.
Ensure personnel training records link directly to role-specific procedures. Keep environmental monitoring, equipment calibration, and maintenance logs current and audit-ready.
Strategic Services in Healthcare Product Development
You will get targeted regulatory planning, compliance pathways, and post-market risk controls to move products from concept to sustained market presence. The guidance focuses on submission strategy, evidence generation, labeling, and lifecycle safety monitoring tailored to your product type and markets.
Regulatory Strategy for Medical Devices
You need a clear device classification and predicate analysis to determine whether to pursue PMA, 510(k), De Novo, or EUA pathways. Identify the device’s intended use, indications, and technological characteristics; this drives the required preclinical testing, bench studies, and clinical evidence.
Create a regulatory roadmap with milestones: pre-submission meetings with the FDA, IDE planning (if clinical data are required), pivotal study design, and submission packaging (e.g., 510(k) summary or PMA modules). Develop a risk management file (ISO 14971) and link it to verification/validation protocols.
Prepare labeling and IFU early; human factors testing results often determine usability-related modifications. Consider combination product designation and consult with Office of Combination Products to set primary jurisdiction and lead review division.
Pharmaceutical Product Compliance
You must define the regulatory pathway—ANDA, 505(b)(2), or full NDA—based on innovator reliance, formulation differences, and clinical bridging needs. Conduct gap analyses against FDA guidances for clinical pharmacology, bioavailability, and stability to scope studies and dossier content.
Assemble the Chemistry, Manufacturing, and Controls (CMC) package with validated analytical methods, process validation data, and facility GMP readiness. Plan for pharmacovigilance infrastructure and Risk Evaluation and Mitigation Strategies (REMS) if the molecule has known serious risks.
Engage the FDA through Type A/B/C meetings to align on clinical endpoints, pediatric plans, and statistical methods. Map out eCTD submission structure, including module assignments and controlled vocabularies, to reduce review cycles.
Post-Market Surveillance Considerations
You should implement a proactive post-market plan that integrates adverse event reporting, trending, and signal detection. Define roles and timelines for MDR/MAUDE reporting, periodic safety updates, and expedited notifications for emerging serious risks.
Set up routine post-approval study commitments, post-market clinical follow-up (PMCF), and real-world evidence (RWE) collection strategies. Use predefined metrics—reporting rates, root-cause analysis frequency, and corrective action timelines—to measure safety performance.
Maintain complaint handling, CAPA, and device master record updates to demonstrate continuous compliance during inspections. Prepare periodic regulatory intelligence reviews to capture labeling, recall, and guidance changes that affect your obligations and market strategy.